https://www.youtube.com/watch?v=NFKHG5pB68I
JENN STARK: Buteyko Method USA-Buteyko Breathing Educators
Posted in General.
Comments Off on JENN STARK: Buteyko Method USA-Buteyko Breathing Educators
– October 28, 2011
Scanning Electron Microscope (SEM) images of plant cell microparticles in urine sediment
Also see:
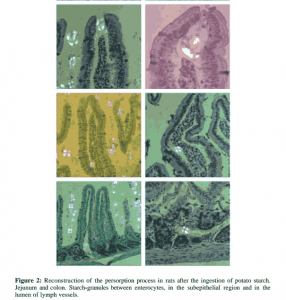
THE PHENOMENON OF PERSORPTION: PERSORPTION, DISSEMINATION, AND ELIMINATION OF MICROPARTICLES
Posted in General.
Comments Off on Scanning Electron Microscope (SEM) images of plant cell microparticles in urine sediment
– October 22, 2011
THE PHENOMENON OF PERSORPTION: PERSORPTION, DISSEMINATION, AND ELIMINATION OF MICROPARTICLES
THE PHENOMENON OF PERSORPTION: PERSORPTION,
DISSEMINATION, AND ELIMINATION OF MICROPARTICLES
by Prof. GERHARD VOLKHEIMER
Solid microparticles, whose diameter lies far in the micrometer range (µm), such as pollen, spores, starch-granules, cellulose particles, silicates, crystals, diatoms, soot particles and other natural and industrial dusts are regularly incorporated in a noteworthy quantity in the alimentary tract. Their paracellular translocation through transitory leaks in the epithelial cell layer has been confirmed. Mechanical factors play an important role here: The solidity of the microparticles, the constantly hammering vascular pulsation communicated to the mucosa and the motility of the muscularis propria and muscularis mucosae are causal factors for the loosening of tight junctions and for the appearance of leaks in the epithelial cell layer. The microparticles are transported from the sub-epithelial region through lymph tracts via the thoracic duct but also through veins and disseminated with the blood stream. They are to be found in the peripheral blood already within a few minutes of peroral application.
There are numerous ways in which the microparticles can be eliminated from the blood stream. Their passage into the alveolar lumen, bile, urine, cerebrospinal fluid, peritoneal cavity, through the lactating mamma into the milk and also the transplacental transfer to the foetal blood circulation has been observed. Numerous ready-to-serve foods contain large quantities of solid microparticles capable of persorption.
“The persorption of microparticles is an effect that may be constantly observed in the passage of food through the organism. The embolisation of small vessels by persorbed particles is of interest from the viewpoint of micro-angiology. The long-term deposition of microparticles that are capable of embolisation and consist of potential allergens or contain contaminants is of immunological and toxicological importance. Environmental and industrial medicine is addressed since industrial and natural dusts passing via the nasopharynx to the alimentary tract are persorbed. A noteworthy observation is the passage via the placenta of persorbed microparticles into the foetal circulation.The phenomenon of the persorption of microparticles still requires numerous supplementary studies; the heuristic value has by no means been exhausted as yet.”
Quotes by Ray Peat, PhD:
“Persorption refers to a process in which relatively large particles pass through the intact wall of the intestine and enter the blood or lymphatic vessels. It can be demonstrated easily, but food regulators prefer to act as though it didn’t exist. The doctrine that polymers–gums, starches, peptides, polyester fat substitutes–and other particulate substances can be safely added to food because they are “too large to be absorbed” is very important to the food industry and its shills.
When the bowel is inflamed, toxins are absorbed. The natural bacterial endotoxin produces many of the same inflammatory effects as the food additive, carrageenan. Like inflammatory bowel disease, the incidence of liver tumors and cirrhosis has increased rapidly. Liver damage leads to hormonal imbalance. Carrageenan produces inflammation and immunodeficiency, synergizing with estrogen, endotoxin and unsaturated fatty acids.”
“Volkheimer found that mice fed raw starch aged at an abnormally fast rate, and when he dissected the starch-fed mice, he found a multitude of blocked arterioles in every organ, each of which caused the death of the cells that depended on the blood supplied by that arteriole. It isn’t hard to see how this would affect the functions of organs such as the brain and heart, even without considering the immunological and other implications….”
“Tiny particles of insoluble materials — clay, starch, soot, bacteria — are all potential sources of serious inflammatory reactions, and the ultra-small particles are potentially ultra-numerous and harder to avoid.”
“Around 1988 I read Gerhard Volkheimer’s persorption article, and after doing some experiments with tortillas and masa, I stopped eating all starch except for those, then eventually I stopped those. Besides grains of starch entering the blood stream, lymph, and cerebral spinal fluid, starch feeds bacteria, increasing endotoxin and serotonin.”
Pathologe. 1993 Sep;14(5):247-52.
[Persorption of microparticles].
[Article in German]
Volkheimer G.
Solid, hard microparticles, such as starch granules, pollen, cellulose particles, fibres and crystals, whose diameters are well into the micrometre range, are incorporated regularly and in considerable numbers from the digestive tract. Motor factors play an important part in the paracellular penetration of the epithelial cell layer. From the subepithelial region the microparticles are transported away via lymph and blood vessels. They can be detected in body fluids using simple methods: only a few minutes after oral administration they can be found in the peripheral blood-stream. We observed their passage into urine, bile, cerebrospinal fluid, the alveolar lumen, the peritoneal cavity, breast milk, and transplacentally into the fetal blood-stream. Since persorbed microparticles can embolise small vessels, this touches on microangiological problems, especially in the region of the CNS. The long-term deposit of embolising microparticles which consist of potential allergens or contaminants, or which are carriers of contaminants, is of immunological and environmental-technical importance. Numerous ready-made foodstuffs contain large quantities of microparticles capable of persorption.
Environ Health Perspect. 1974 Dec;9:215-25.
Passage of particles through the wall of the gastrointestinal tract.
Volkheimer G.
In the normal process of digestion, not only substances in solution are absorbed. Solid, undissolved particles in macrocorpuscular form, are “kneaded” into the mucosa during their passage through the digestive tract. These particles in the micrometer size range pass between the epithelial cells into the subepithelial layer. From here they are transmitted both by the lymph vessels and by the mesenteric veins into the circulation, where they remain for a considerable time. This phenomenon, termed persorption, was investigated in detail.
Med Hypotheses. 1991 Jun;35(2):85-7.
Persorption of raw starch: a cause of senile dementia?
Freedman BJ.
Intact starch granules in food can pass through the intestinal wall and enter the circulation. They remain intact if they have not been cooked for long enough in the presence of water. Some of these granules embolise arterioles and capillaries. In most organs the collateral circulation suffices for continued function. In the brain, however, neurones may be lost. Over many decades the neuronal loss could be of clinical importance. To test this hypothesis, there is a need to examine brains for the presence of embolised starch granules. Examining tissues polariscopically clearly distinguishes starch granules from other objects of similar appearance.
Dig Dis Sci. 1995 May;40(5):967-75.
Uptake and translocation of microparticles in small intestine. Morphology and quantification of particle distribution.
Hodges GM, Carr EA, Hazzard RA, Carr KE.
The intestinal transit of large (micro-) particles to other sites of the body remains a controversial issue of relevance in various fields of study. In this report fluorescent polystyrene latex microparticles in the size range of 2 microns were used as models for nonspecifically absorbed nonbiodegradable particulates. They were administered to young adult rats as a single oral dose of 1.65 x 10(9) particles; Peyer’s patches and surrounding normal absorptive small intestinal tissue were collected at various time points. Quantification of solubilized tissue samples and fluorescence (epi- and confocal) qualitative and quantitative microscopy showed uptake of latex microparticles in all parts of the intestine sampled, but with the proximal segment the preferential site of absorption. The maximum uptake of particles occurred 0.5 hr after dosing in all three segments of the small intestine; there were progressively smaller numbers with distance from the pylorus and with time. Translocation of small numbers of particles to the mesenteric lymph nodes was also detected at 0.5 hr. Transmucosal passage of particles occurred primarily in the villous tissues adjacent to the Peyer’s patch regions. These studies give confirmatory evidence for the uptake and translocation of microparticulates across the mucosal barrier and provide new information regarding site- and time-related effects on particle uptake and the involvement of the villous epithelium in particle translocation.
J Anat. 1996 Oct;189 ( Pt 2):265-71.
Early intestinal microparticle uptake in the rat.
Hazzard RA, Hodges GM, Scott JD, McGuinness CB, Carr KE.
This time-course study investigates the early uptake and passage of microparticles across the intestinal mucosa. Single intraoral doses of fluorescent latex particles, 1.82 microns in diameter, were administered to young adult male, nonfasted rats at a dose of 1.88 x 10(9) particles. Peyer’s patch regions and mesenteric lymph nodes were collected at 5, 15 and 30 min time points for both bulk tissue and morphological analyses. Particles were found at all experimental time points in macerated intestinal and nodal specimens: particle numbers were higher in proximal than in distal intestine at all time points despite the fact that particle numbers in distal Peyer’s patch regions increased with time. Particle numbers in mesenteric lymph nodes also increased with time after administration. Detailed morphological data for several intestinal and nodal tissue compartments showed substantial early uptake of particles by villous epithelium, including goblet cells, but low involvement of follicle-associated cells. The distribution of particles in the lymph nodes confirmed that translocation occurred to all nodal compartments. These studies give confirmatory evidence that uptake and translocation of microparticles may take place as early as 5 min after administration and suggest that intestinal region may influence uptake.
Posted in General.
Comments Off on THE PHENOMENON OF PERSORPTION: PERSORPTION, DISSEMINATION, AND ELIMINATION OF MICROPARTICLES
– October 22, 2011
A Reply to Ray Peat on Essential Fatty Acid Deficiency
Ray Peat, PhD, is an influential health writer who claims that there is no such thing as essential fatty acid (EFA) deficiency. According to Peat, the body can make its own EFAs; furthermore, he claims that EFAs in the body become rancid and therefore cause cancer.
Unfortunately, Peat does not understand the use of EFA by the human body. He is trained in hormone therapy and his training in fats and oils has been limited to misinformation as far as the polyunsaturated fats and oils are concerned.
Research on EFAs is voluminous and consistent: EFAs are types of fatty acids that the body cannot make, but must obtain from food. We do not make them because they exist in virtually all foods, and the body needs them only in small amounts. The body does make saturated and monounsaturated fatty acids because it needs these in large amounts and cannot count on getting all it needs from food.
There are two types of EFAs, those of the omega-6 family and those of the omega-3 family. The basic omega-6 fatty acid is called linoleic acid and it contains two double bonds. It is found in virtually all foods, but especially in nuts and seeds. The basic omega-3 fatty acid is called linolenic acid and it contains three double bonds. It is found in some grains (such as wheat) and nuts (such as walnuts) as well as in eggs, organ meats and fish if these animals are raised naturally, and in green vegetables if the plants are raised organically.
Essential fatty acids have two principal roles. The first is as a constituent of the cell membrane. Each cell in the body is surrounded by a membrane composed of billions of fatty acids. About half of these fatty acids are saturated or monounsaturated to provide stability to the membrane. The other half are polyunsaturated, mostly EFAs , which provide flexibility and participate in a number of biochemical processes. The other vital role for EFAs is as a precursor for prostaglandins or local tissue hormones, which control different physiological functions including inflammation and blood clotting.
Scientists have induced EFA deficiency in animals by feeding them fully hydrogenated coconut oil as their only fat. (Full hydrogenation gets rid of all the EFAs; coconut oil is used because it is the only fat that can be fully hydrogenated and still be soft enough to eat.) The animals developed dry coats and skin and slowly declined in health, dying prematurely. (Interestingly, representatives of the vegetable oil industry blame the health problems on coconut oil, not on fatty acid deficiency!)
In a situation of fatty acid deficiency, the body tries to compensate by producing a fatty acid called Mead acid out of the monounsaturated oleic acid. It is a 20-carbon fatty acid with three double bonds named after James Mead, a lipids researcher at the University of California at Los Angeles who first identified it. An elevated level of Mead acid in the body is a marker of EFA deficiency.
According to Peat, elevated levels of Mead acid constitute proof that your body can make EFAs. However, the Mead acid acts as a “filler” fatty acid that cannot serve the functions that the original EFA are needed for. Peat claims that Mead acid has a full spectrum of protective anti-inflammatory effects; however, the body cannot convert Mead acid into the elongated fatty acids that the body needs for making the various anti-inflammatory prostaglandins.
Peat also asserts that polyunsaturated fatty acids become rancid in our bodies. This is not true; the polyunsaturated fatty acids in our cell membranes go through different stages of controlled oxidation. To say that these fatty acids become “rancid” is misleading. Of course, EFAs can become rancid through high temperature processing and it is not healthy to consume these types of fats. But the EFAs that we take in through fresh, unprocessed food are not rancid and do not become rancid in the body. In small amounts, they are essential for good health. In large amounts, they can pose health problems which is why we need to avoid all the commercial vegetable oils containing high levels of polyunsaturates.
Peat’s reasoning has led him to claim that cod liver oil causes cancer because cod liver oil contains polyunsaturated fatty acids. Actually, the main fatty acid in cod liver oil is a monounsaturated fatty acid. The two main polyunsaturated fatty acids in cod liver oil are the elongated omega-3 fatty acids called EPA and DHA, which play many vital roles in the body and actually can help protect against cancer. Furthermore, cod liver oil is our best dietary source of vitamins A and D, which also protect us against cancer.
Actually, Peat’s argument that polyunsaturated fatty acids become harmful in the body and hence cause cancer simply does not make sense. It is impossible to avoid polyunsaturated fatty acids because they are in all foods.
EFAs are, however, harmful in large amounts and the many research papers cited by Peat showing immune problems, increased cancer and premature aging from feeding of polyunsaturates simply corroborate this fact. But Peat has taken studies indicating that large amounts of EFAs are bad for us (a now well-established fact) and used them to argue that we don’t need any at all.
Finally, it should be stressed that certain components of the diet actually reduce (but do not eliminate) our requirements for EFAs. The main one is saturated fatty acids which help us conserve EFAs and put them in the tissues where they belong. Some studies indicate that vitamin B6 can ameliorate the problems caused by EFA deficiency, possibly by helping us use them more efficiently.
This article appeared in Wise Traditions in Food, Farming and the Healing Arts, the quarterly magazine of the Weston A. Price Foundation, Spring 2005.
About the Author

Mary G. Enig, PhD is an expert of international renown in the field of lipid biochemistry. She has headed a number of studies on the content and effects of trans fatty acids in America and Israel, and has successfully challenged government assertions that dietary animal fat causes cancer and heart disease. Recent scientific and media attention on the possible adverse health effects of trans fatty acids has brought increased attention to her work. She is a licensed nutritionist, certified by the Certification Board for Nutrition Specialists, a qualified expert witness, nutrition consultant to individuals, industry and state and federal governments, contributing editor to a number of scientific publications, Fellow of the American College of Nutrition and President of the Maryland Nutritionists Association. She is the author of over 60 technical papers and presentations, as well as a popular lecturer. Dr. Enig is currently working on the exploratory development of an adjunct therapy for AIDS using complete medium chain saturated fatty acids from whole foods. She is Vice-President of the Weston A Price Foundation and Scientific Editor of Wise Traditions as well as the author of Know Your Fats: The Complete Primer for Understanding the Nutrition of Fats, Oils, and Cholesterol, Bethesda Press, May 2000. She is the mother of three healthy children brought up on whole foods including butter, cream, eggs and meat.
Posted in General.
rev="post-3153" 3 comments
– October 21, 2011
Chronic hyperventilation; have you got it, what is it, and how do you fix it?
By Dr Janet Winter, Posted on July 28, 2011
The consequences of chronic hyperventilation or over breathing can be many; tired muscles, headaches, anxiety, poor sleep, fatigue, allergies, cold hands, breathlessness, stuffed nose, IBS…. The list goes on.
One definition of hyperventilation is breathing more than your body requires, so if you are sitting, but breathing as if you were running, that is hyperventilation.
But that’s not a problem is it? The more oxygen the better, no? Unfortunately not. There is nearly 10 times more oxygen than we need in the air we breathe, so it is really easy to get enough into our blood and get 98% saturation of haemoglobin, the protein in red blood cells that transports oxygen.
The problem comes when we flush out too much carbon dioxide by breathing too much; it’s not just a waste gas, but we need high amounts in our tissues, and as there is very little in the air we breathe, we can flush it out by breathing too much. (And we don’t get much more oxygen for our trouble, as you can’t get more than 100%!) In fact another definition of hyperventilation is by measuring blood gases and finding an abnormally low amount of carbon dioxide.
Well why do we need that carbon dioxide? Imagine that you have lots of oxygen in your blood stream. The blood supplies all the body tissues with this oxygen, but there has to be a mechanism to release that oxygen in the right amount, in the correct place, i.e in the tissues that need it most – the ones doing most work. And what do the hard working tissues release? Carbon dioxide. Yes it is carbon dioxide that is the signal from those hard working muscles etc that more oxygen is needed. So the high amounts of carbon dioxide in active tissues, trigger oxygen release from haemoglobin on red blood cells, and drive it out of the bloodstream to where it is required.
The problems arise when too much carbon dioxide is flushed from the system, and oxygen cannot be released efficiently from the bloodstream to the tissues that need it. So THE MORE YOU BREATHE THE LESS OXYGEN YOU GET! This is a very well documented effect, the Bohr effect.
So hyperventilation: tired muscles, headaches, anxiety, poor sleep, fatigue, allergies, cold hands, breathlessness, stuffed nose, IBS…. Do you recognise any of them?
The news doesn’t get any better, as this chronic hyperventilation is also known as hidden hyperventilation, and is unlikely to be recognised by your GP. Over the years you may collect more symptoms, with increased severity.
But the good news is that once you recognise it, you can put right this hyperventilation, and gently correct your breathing, often watching your troublesome symptoms dissolve away as you do.
This is what a Buteyko practitioner can help you with.
Find out more at www.BreathingRemedies.co.uk
Source:
http://blog.naturaltherapyforall.com/2011/07/28/chronic-hyperventilation-have-you-got-it-what-is-it-and-how-do-you-fix-it/
Posted in General.
Comments Off on Chronic hyperventilation; have you got it, what is it, and how do you fix it?
– October 21, 2011
Bohr Effect and Cells O2 Levels: Healthy vs. Sick People
Carbon dioxide (CO2) is the key player in O2 transport due to 1) vasodilation and 2) the the Bohr effect (or the Bohr law). The Bohr effect explains oxygen release in capillaries or why red blood cells unload oxygen in tissues. The Bohr effect was first described in 1904 by the Danish physiologist Christian Bohr (father of famous physicist Niels Bohr). Christian Bohr stated that at lower pH (more acidic environment, e.g., in tissues), hemoglobin will bind to oxygen with less affinity. Since carbon dioxide is in direct equilibrium with the concentration of protons in the blood, increasing blood carbon dioxide content causes a decrease in pH, which leads to a decrease in affinity for oxygen by hemoglobin (and easier oxygen release in capillaries).
The description of this physiological law can be found in standard physiological textbooks. Modern studies in this area are devoted to more advanced topics (e.g., Braumann et al, 1982; Böning et al, 1975; Bucci et al, 1985; Carter et al, 1985; diBella et al, 1986; Dzhagarov et al, 1996; Grant et al, 1982; Grubb et al, 1979;  Gersonde et al, 1986; Hlastala & Woodson, 1983; Jensen, 2004; Kister et al, 1988; Kobayashi et al, 1989; Lapennas, 1983; Matthew et al, 1979; Meyer et al, 1978; Tyuma, 1984; Winslow et al, 1985). It is the central proposition of this law that oxygen affinity to hemoglobin depends on absolute CO2 concentrations and reduced CO2 values decrease cells oxygen content.
Gersonde et al, 1986; Hlastala & Woodson, 1983; Jensen, 2004; Kister et al, 1988; Kobayashi et al, 1989; Lapennas, 1983; Matthew et al, 1979; Meyer et al, 1978; Tyuma, 1984; Winslow et al, 1985). It is the central proposition of this law that oxygen affinity to hemoglobin depends on absolute CO2 concentrations and reduced CO2 values decrease cells oxygen content.
What is the Bohr effect in simple terms?
As we know, oxygen is transported in blood by hemoglobin cells. How do these red blood cells know where to release more oxygen and where less? Or why do they unload more oxygen at all? Why is O2 released in tissues? The hemoglobin cells sense higher concentrations of CO2 in tissues and release oxygen in such places.
Conclusion. More oxygen is released in those tissues
that have higher absolute and/or relative CO2 values.
This is true for healthy people who have normal breathing pattern. What about person with chronic diseases?
Minute ventilation rates (chronic diseases)
| Condition | Minute ventilation |
Number of people |
All references or click below for abstracts |
| Normal breathing | 6 L/min | – | Medical textbooks |
| Healthy Subjects | 6-7 L/min | >400 | Results of 14 studies |
| Heart disease | 15 (±4) L/min | 22 | Dimopoulou et al, 2001 |
| Heart disease | 16 (±2) L/min | 11 | Johnson et al, 2000 |
| Heart disease | 12 (±3) L/min | 132 | Fanfulla et al, 1998 |
| Heart disease | 15 (±4) L/min | 55 | Clark et al, 1997 |
| Heart disease | 13 (±4) L/min | 15 | Banning et al, 1995 |
| Heart disease | 15 (±4) L/min | 88 | Clark et al, 1995 |
| Heart disease | 14 (±2) L/min | 30 | Buller et al, 1990 |
| Heart disease | 16 (±6) L/min | 20 | Elborn et al, 1990 |
| Pulm hypertension | 12 (±2) L/min | 11 | D’Alonzo et al, 1987 |
| Cancer | 12 (±2) L/min | 40 | Travers et al, 2008 |
| Diabetes | 12-17 L/min | 26 | Bottini et al, 2003 |
| Diabetes | 15 (±2) L/min | 45 | Tantucci et al, 2001 |
| Diabetes | 12 (±2) L/min | 8 | Mancini et al, 1999 |
| Diabetes | 10-20 L/min | 28 | Tantucci et al, 1997 |
| Diabetes | 13 (±2) L/min | 20 | Tantucci et al, 1996 |
| Asthma | 13 (±2) L/min | 16 | Chalupa et al, 2004 |
| Asthma | 15 L/min | 8 | Johnson et al, 1995 |
| Asthma | 14 (±6) L/min | 39 | Bowler et al, 1998 |
| Asthma | 13 (±4) L/min | 17 | Kassabian et al, 1982 |
| Asthma | 12 L/min | 101 | McFadden & Lyons, 1968 |
| COPD | 14 (±2) L/min | 12 | Palange et al, 2001 |
| COPD | 12 (±2) L/min | 10 | Sinderby et al, 2001 |
| COPD | 14 L/min | 3 | Stulbarg et al, 2001 |
| Sleep apnea | 15 (±3) L/min | 20 | Radwan et al, 2001 |
| Liver cirrhosis | 11-18 L/min | 24 | Epstein et al, 1998 |
| Hyperthyroidism | 15 (±1) L/min | 42 | Kahaly, 1998 |
| Cystic fibrosis | 15 L/min | 15 | Fauroux et al, 2006 |
| Cystic fibrosis | 10 L/min | 11 | Browning et al, 1990 |
| Cystic fibrosis* | 10 L/min | 10 | Ward et al, 1999 |
| CF and diabetes* | 10 L/min | 7 | Ward et al, 1999 |
| Cystic fibrosis | 16 L/min | 7 | Dodd et al, 2006 |
| Cystic fibrosis | 18 L/min | 9 | McKone et al, 2005 |
| Cystic fibrosis* | 13 (±2) L/min | 10 | Bell et al, 1996 |
| Cystic fibrosis | 11-14 L/min | 6 | Tepper et al, 1983 |
| Epilepsy | 13 L/min | 12 | Esquivel et al, 1991 |
| CHV | 13 (±2) L/min | 134 | Han et al, 1997 |
| Panic disorder | 12 (±5) L/min | 12 | Pain et al, 1991 |
| Bipolar disorder | 11 (±2) L/min | 16 | MacKinnon et al, 2007 |
| Dystrophia myotonica | 16 (±4) L/min | 12 | Clague et al, 1994 |
Overbreathing or hyperventilation in the sick (with exception for those who have problems with lungs and ventilation-perfusion mismatch) causes hypocapnia or reduced CO2 tissue tension in the lungs and arterial blood (ventilation-perfusion mismatch is not a common finding in the sick). This leads to hampered oxygen release and reduced cells oxygen tension (Aarnoudse et al, 1981; Monday & Tétreault, 1980; Gottstein et al, 1976).
Hence, if absolute CO2 concentration is low (see the picture of the right side), O2 molecules are stuck with red blood cells. (Scientists call this effect “increased oxygen affinity to hemoglobin”). Hence, CO2 deficiency (hypocapnia) leads to hypoxia or cells oxygen levels (the suppressed Bohr effect). The more we breathe at rest, the less the amount of available oxygen in the cells of vital organs, like brain, heart, liver, kidneys, etc.
Hemoglobin cells in normal blood are about 98% saturated with O2. When we hyperventilate this number is about the same (in best case, since transition to costal or chest breathing reduces arterial blood O2 levels), but without CO2, this oxygen is tightly bound with red blood cells and cannot get into the tissues in required amounts. Hence, now we know one of the causes why heavy breathing reduces cell oxygen level of all vital organs.
 The Bohr effect is crucial for our survival. Why? During each moment of our lives, some organs and tissues work harder and produce more CO2. These additional CO2 concentrations are sensed by the hemoglobin cells and cause them to release more O2 in those places where it is most required. This is a smart self-regulating mechanism for efficient cells oxygen transport.
The Bohr effect is crucial for our survival. Why? During each moment of our lives, some organs and tissues work harder and produce more CO2. These additional CO2 concentrations are sensed by the hemoglobin cells and cause them to release more O2 in those places where it is most required. This is a smart self-regulating mechanism for efficient cells oxygen transport.
Bohr effect and physical exercise
For example, without the Bohr effect, you could not walk or run for even 3-5 minutes. Why? In normal conditions, due to the Bohr effect, more O2 is released in those muscles, which generate more CO2. Hence, these muscles can continue to work with the same high rate.
However, sick people have reduced CO2 blood values. Hence, they are likely to experience symptoms of chronic fatigue due to tissue hypoxia (low cells oxygen levels).
“But even as early as 1885, Miescher (Swiss physiologist) inspired by the insight of genius wrote: “Over the O2 supply of the body, CO2 spreads its protecting wings” Yandell Henderson (1873-1944), in Henderson Y, Carbon dioxide, in Cyclopedia of Medicine, ed. by HH Young, Philadelphia, FA Davis, 1940.
Here is YouTube video that considers the Bohr effect and explains the mechanism why overbreathing decreases cells oxygen level.
Another web page related to oxygen transport and cell oxygenation: Vasodilation (expansion of arteries and arterioles due to higher CO2 values) or why breathing less improves perfusion and oxygenation of all vital organs.
You can read medical research abstract devoted to the Bohr effect and role of CO2 in cells O2 delivery.
References (abstracts are below)
Aarnoudse JG, Oeseburg B, Kwant G, Zwart A, Zijlstra WG, Huisjes HJ, Influence of variations in pH and PCO2 on scalp tissue oxygen tension and carotid arterial oxygen tension in the fetal lamb, Biol Neonate 1981; 40(5-6): p. 252-263.
Braumann KM, Böning D, Trost F, Bohr effect and slope of the oxygen dissociation curve after physical training, J Appl Physiol. 1982 Jun; 52(6): p. 1524-1529.
Böning D, Schwiegart U, Tibes U, Hemmer B, Influences of exercise and endurance training on the oxygen dissociation curve of blood under in vivo and in vitro conditions, Eur J Appl Physiol Occup Physiol. 1975; 34(1): p. 1-10.
Bucci E, Fronticelli C, Anion Bohr effect of human hemoglobin, Biochemistry. 1985 Jan 15; 24(2): p. 371-376.
Carter AM, Grønlund J, Contribution of the Bohr effect to the fall in fetal PO2 caused by maternal alkalosis, J Perinat Med. 1985; 13(4): p.185-191.
diBella G, Scandariato G, Suriano O, Rizzo A, Oxygen affinity and Bohr effect responses to 2,3-diphosphoglycerate in equine and human blood, Res Vet Sci. 1996 May; 60(3): p. 272-275.
Dzhagarov BM, Kruk NN, The alkaline Bohr effect: regulation of O2 binding with triliganded hemoglobin Hb(O2)3 [Article in Russian] Biofizika. 1996 May-Jun; 41(3): p. 606-612.
Gersonde K, Sick H, Overkamp M, Smith KM, Parish DW, Bohr effect in monomeric insect haemoglobins controlled by O2 off-rate and modulated by haem-rotational disorder, Eur J Biochem. 1986 Jun 2; 157(2): p. 393-404.
Grant BJ, Influence of Bohr-Haldane effect on steady-state gas exchange, J Appl Physiol. 1982 May; 52(5): p. 1330-1337.
Grubb B, Jones JH, Schmidt-Nielsen K, Avian cerebral blood flow: influence of the Bohr effect on oxygen supply, Am J Physiol. 1979 May; 236(5): p. H744-749.
Gottstein U, Zahn U, Held K, Gabriel FH, Textor T, Berghoff W, Effect of hyperventilation on cerebral blood flow and metabolism in man; continuous monitoring of arterio-cerebral venous glucose differences (author’s transl) [Article in German], Klin Wochenschr. 1976 Apr 15; 54(8): p. 373-381.
Hlastala MP, Woodson RD, Bohr effect data for blood gas calculations, J Appl Physiol. 1983 Sep; 55(3): p. 1002-1007.
Jensen FB, Red blood cell pH, the Bohr effect, and other oxygenation-linked phenomena in blood O2 and CO2 transport, Acta Physiol Scand. 2004 Nov; 182(3): p. 215-227.
Kister J, Marden MC, Bohn B, Poyart C, Functional properties of hemoglobin in human red cells: II. Determination of the Bohr effect, Respir Physiol. 1988 Sep; 73(3): p. 363-378.
Kobayashi H, Pelster B, Piiper J, Scheid P, Significance of the Bohr effect for body oxygen level in a model with counter-current blood flow, Respir Physiol. 1989 Jun; 76(3): p. 277-288.
Lapennas GN, The magnitude of the Bohr coefficient: optimal for oxygen delivery, Respir Physiol. 1983 Nov; 54(2): p.161-172.
Matthew JB, Hanania GI, Gurd FR, Electrostatic effects in hemoglobin: Bohr effect and ionic strength dependence of individual groups, Biochemistry. 1979 May 15; 18(10): p.1928-1936.
Meyer M, Holle JP, Scheid P, Bohr effect induced by CO2 and fixed acid at various levels of O2 saturation in duck blood, Pflugers Arch. 1978 Sep 29; 376(3): p. 237-240.
Monday LA, Tétreault L, Hyperventilation and vertigo, Laryngoscope 1980 Jun; 90(6 Pt 1): p.1003-1010.
Tyuma I, The Bohr effect and the Haldane effect in human hemoglobin, Jpn J Physiol. 1984; 34(2): p.205-216.
Winslow RM, Monge C, Winslow NJ, Gibson CG, Whittembury J, Normal whole blood Bohr effect in Peruvian natives of high altitude, Respir Physiol. 1985 Aug; 61(2): p. 197-208.
http://www.normalbreathing.com/CO2-bohr-effect.php
Posted in General.
Comments Off on Bohr Effect and Cells O2 Levels: Healthy vs. Sick People
– October 20, 2011
Hormone Balancing: Natural Treatment and Cure for Arthritis
Also see:
Arthritis and Hypothyroidism
by Raymond F. Peat, Ph.D.
Medical data is for informational purposes only. You should always consult your family physician, or one of our referral physicians prior to treatment.
(Formerly published in The Journal of the Rheumatoid Disease
Foundation, Volume 1, Number 1), The Roger Wyburn-Mason and Jack M.
Blount Foundation for the Eradication of Rheumatoid Disease
AKA The Arthritis Trust of America®,
7376 Walker Road, Fairview, TN 37062
Copyright 1986
A very healthy 71-year-old man was under his house repairing
the foundation, when a support slipped and let the house fall far
enough to break some facial bones. During his recovery, he devel-
oped inflammatory arthritis in his hands. It is fairly common for
arthritis to appear shortly after an accident, a shock, or surgery, and
Hans Selye’s famous work with rats shows that when stress ex-
hausts the adrenal glands (so they are unable to produce normal
amounts of cortisone and related steroid hormones), osteoarthritis
and other “degenerative” diseases are likely to develop. But when
this man went to his doctor to “get something for his arthritis,” he
was annoyed that the doctor insisted on giving him a complete physi-
cal exam, and wouldn’t give him a shot of cortisone. The laboratory
examination showed low thyroid function, and the doctor prescribed
a supplement of thyroid extract, explaining that arthritis is one of the
many symptoms of hypothyroidism. The patient agreed to take the
thyroid, but for several days he grumbled about the doctor “fixing
something that wasn’t wrong” with him, and ignoring his arthritis.
But in less than two weeks, the arthritis had entirely disappeared. He
lived to be 88, but without a recurrence of arthritis. (See “Thyroid
Hormone Therapy: Cutting the Gordian Knot,” and “Stress,” http://
www.arthritistrust.org.)
Selye’s work with the diseases of stress, and the anti-stress
hormones of the adrenal cortex, helped many scientists to think more
clearly about the interaction of the organism with its environment,
but it has led others to focus too narrowly on hormones of the
adrenal cortex (such as cortisol and cortisone), and to forget the older
knowledge about natural resistance. There are probably only a few
physicians now practicing who would remember to check for hy-
pothyroidism in an arthritis patient, or in other stress-related condi-
tions. Hypothyroidism is a common cause of adrenal insufficiency,
but it also has some direct effects on the joint tissues. In chronic
hypothyroidism (myxedema and cretinism), knees and elbows are
often bent abnormally.
By the 1930s, it was well established that the resistance of the
organism depended on the energy produced by respiration under the
influence of the thyroid gland, as well as on the adrenal hormones,
and that the hormones or pregnancy (especially progesterone) could
substitute for the adrenal hormones. In a sense, the thyroid hormone
is the basic anti-stress hormone, since it is required for the produc-
tion of the adrenal and pregnancy hormones. A contemporary re-
searcher, F.Z. Meerson1, is putting together a picture of the biologi-
cal processes involved in adapting to stress, including energy pro-
duction, nutrition, hormones, and changes in cell structure.
While one of Selye’s earliest observations related gastro-intes-
tinal bleeding to stress, Meerson’s work has revealed in a detailed
way how the usually beneficial hormone of adaptation, cortisone,
can cause so many other harmful effects when its action is too pro-
longed or too intense.
Some of the harmful effects of the cortisone class of drugs
(other than gastro-intestinal bleeding) are: Hypertension, Osteoporo-
sis, delayed healing, atrophy of the skin, convulsions, cataracts, glau-
coma, protruding eyes, psychic derangements, menstrual irregulari-
ties, and loss of immunity allowing infections or cancer to spread.
While normal thyroid function is required for the secretion of
the adrenal hormones, the basic signal which causes cortisone to be
formed is a drop in the blood glucose level. The increased energy
requirement of any stress tends to cause the blood sugar to fall
slightly, but hypothyroidism itself tends to depress blood sugar. The
person with low thyroid function is more likely than a normal person
to require cortisone to cope with a certain amount of stress. How-
ever, if large amounts of cortisone are produced for a long time, the
toxic effects of the hormone begin to appear. According to Meerson,
heart attacks are provoked and aggravated by cortisone produced
during stress. (Meerson and his colleagues have demonstrated that
the progress of a heart attack can be halted by a treatment including
natural substances such as vitamin E and magnesium.)
While hypothyroidism makes the body require more cortisone
to sustain blood sugar and energy production, it also limits the ability
to produce cortisone, so in some cases stress produces symptoms
resulting from a deficiency of cortisone, including various forms of
arthritis and more generalized types of chronic inflammation. Since
cortisol is formed as one of the last steps in a series of reactions,
glandular exhaustion means that a whole group of other steroids is
depleted, before cortisol or cortisone. I believe that the safest way to
handle a steroid deficiency is to supplement the precursors of the raw
materials, so that a normal balance of the various substances is pre-
served.
Often, a small physiological dose of natural hydrocortisone can
help the patient meet the stress, without causing harmful side effects.
While treating the symptoms with cortisone for a short time, it is
important to try to learn the basic cause of the problem, by checking
for hypothyroidism, vitamin A deficiency, protein deficiency, a lack
of sunlight, etc. (I suspect that ultraviolet light on the skin directly
increases the skin’s production of steroids, without depending on
other organs.) Using cortisone physiologically, rather than pharma-
cologically, it is not likely to cause the serious problems mentioned
above.
Stress-induced cortisone deficiency is thought to be a factor in
a great variety of unpleasant conditions, from allergies to ulcerative
colitis, and in some forms of arthritis. The stress which can cause a
cortisone deficiency is even more likely to disturb formation of
progesterone and thyroid hormone, so the fact that cortisone can
relieve symptoms does not mean that it has corrected the problem.
Besides the thyroid, the other class of adaptive hormones which
are often out of balance in the diseases of stress, is the group of
hormones produced mainly by the gonads: the “reproductive hor-
mones.” During pregnancy, these hormones serve to protect the
developing baby from the stresses suffered by the mother, but the
same hormones function as a part of the protective anti-stress system
in the non-pregnant individual, though as a lower level.
Some forms of arthritis are known to improve or even to disap-
pear during pregnancy. As mentioned above, the hormones of preg-
nancy can make up for a lack of adrenal cortex hormones. During a
healthy pregnancy, many hormones are present in increased amounts,
including the thyroid hormones. Progesterone, which is the most
abundant hormone of pregnancy, has both anti-inflammatory and
anesthetic actions, which would be of obvious benefit in arthritis.
There are other naturally anesthetic hormones which are increased
during pregnancy, including DHEA, which is being studied for its
anti-aging, anti-cancer, and anti-obesity effects. (One of the reasons
that is frequently given for the fact that this hormone hasn’t been
studied more widely is that, as a natural substance, it has not been
monopolized by a drug patent, and so no drug company has been
willing to invest money in studying its medical uses.) These hor-
mones also have the ability to control cell division, which would be
important in forms of arthritis that involve invasive tissue growth.
While these substances, so abundant in pregnancy, have the
ability to substitute for cortisone, they can also be used by the adrenal
glands to produce cortisol and related hormones. But probably the
most surprising property of these natural steroids is that they protect
against the toxic side-effects of excessive adrenal hormones. And
they seem to have no side-effects of their own; after fifty years of
medical use, no toxic side effects have been found for progesterone
or pregnenolone. Pregnenolone is the material the body uses to form
either progesterone or DHEA. Others, including DHEA, haven’t
been studied for so long, but the high levels which are normally
present in healthy people would suggest that replacement doses, to
restore those normal levels, would not be likely to produce toxic side
effects. And, considering the terrible side effects of the drugs that are
now widely used, these drugs would be justifiable simply to prevent
some of the toxic effects of conventional treatment. It takes a new
way of thinking to understand that these protective substances pro-
tect against an excess of the adrenal steroids, as well as making up
for a deficiency. Several of these natural hormones also have a
protective action against various poisons — Selye called this their
“catatoxic” effect. (If a toxin, for example a bacterial product, is
involved in a sickness, such as arthritis or colitis, these catatoxic
steroids might be helping by blocking the toxin and strengthening
the patient.)
Besides many people whose arthritis improved with only thy-
roid supplementation, I have seen people use one or more of these
other natural hormones for various types of arthritis, usually with a
topical application, and I know of several other people who used
progesterone topically for inflamed tendons or other inflammations.
Only one of these, a woman with rheumatoid arthritis in many joints,
had no significant improvement. An hour after she had applied it to
her hands and feet, she enthusiastically reported that her ankle had
stopped hurting. But after this, she said she had no noticeable im-
provement.
The first time I saw arthritis disappear after treatment with
progesterone was accidental. A woman who began using progester-
one for her epilepsy decided to dip her arthritic fingers in the oily
solution, and a few days later proudly demonstrated that she could
bend them without pain.
About a year later, a friend in Mexico City complained about a
knee that had been increasingly stiff and painful for about a year.
Twenty minutes after applying progesterone the pain was gone, and
when I asked him about it a few years later, he said it never hurt
again. Knowing that those “raw material” steroids, pregnenolone,
progesterone, and DHEA, could be converted into anything the body
needs, such as cortisone and sex hormones, but that they protect
against the toxic effects of other hormones, many other people (in-
cluding physicians and researchers) were interested in trying them
on their own joint problems.
Some typical cases are described below:
1. A 72-year-old woman. She was considered to have mild
rheumatoid arthritis which was degenerating into porosis, with her
fingers being the most seriously affected joints. A 3% solution of
DHEA in olive oil was applied to one index finger, and a 10%
solution of progesterone in mixed tocopherols was applied to the
other index finger. All of her fingers had been rigid for over a year,
with the result that she was extremely disabled. Forty minutes after
the DHEA solution had been applied, the finger treated with that
solution could be bent enough to touch the base of her thumb, with-
out significant pain, but none of her other fingers showed any im-
provement. Several days later, the DHEA solution was applied to all
of her fingers, with similarly good results. After about 6 months,
stiffness and pain returned in spite of her use of DHEA. Although
thyroid was suggested, she had been taught to be afraid of that
hormone, as have millions of other women.
2. A 60-year-old woman with a long history of rheumatoid
arthritis had serious degeneration of many joints. She had under-
gone surgery several times, for implantation of two artificial joints
and for repair of joint cartilage. She walked a little as possible and
experienced pain, inflammation and fatigue with excessive walking.
She applied a solution containing 7% DHEA and 3% progesterone
in a solvent consisting of olive oil and tocopherol. She applied the
solution several times one afternoon and the next morning to all
affected joints, including hands, wrists, elbows, knees, and ankles.
She experienced what she said was “complete relief,” and spent the
next two days walking around the town sightseeing, without any of
the after-effects she had previously experienced from walking.
3. A 62-year-old man. His knees had been stiff, painful, and
inflamed for over two years, following an accidental fall onto his
knees. Arthroscopic examination revealed damaged cartilage in his
right knee, and surgery was recommended to restore function. The
patient refused surgery, even though he walked with difficulty and
had to use his left leg (which was also affected) to lift himself slowly
up steps. He said he had not slept well since he had developed the
arthritis, because the pain woke him repeatedly during the night, and
only the use of an analgesic would allow him to go back to sleep. He
coated his knees and the skin around them, about four inches above
and below, with a total of nearly an ounce of a solution similar to that
used in case number two. Within 30 minutes, he appeared to able to
walk more normally, and about 45 minutes after applying the solu-
tion, he remarked that he believed he was able to walk more easily.
He repeated the application that night before going to sleep. Around
10 o’clock the next morning, he returned and laughingly demon-
strated his knees by running up the stairs, and said that he had been
able to sleep through the night for the first time in years, and had not
taken his usual analgesic. Topical treatment was discontinued after a
few days, and he remained free of symptoms while taking 60 mg of
pregnenolone orally, daily.
4. A 61-year-old woman. Painful and stiff joints in her hands
had interfered with her work as a musician, and had made it impos-
sible to sleep through the night, since the pain woke her two or three
times during the night. A solution similar to that used in cases three
and four was applied to the painful joints early in the evening, and a
few hours later she was able to go to sleep without taking aspirin and
slept through the night. She occasionally uses the same solution
preventatively, and has not had a recurrence of the joint pain or
stiffness.
We often hear that “there is no cure for arthritis, because the
causes are not known.” If the cause is an imbalance in the normal
hormones of adaptation and resistance, then eliminating the cause by
restoring this balance will produce a true cure.
Informed patients who suspect that their health problems are
related to stress should encourage their physicians to investigate the
use of thyroid hormone, progesterone, pregnenolone, DHEA, and
the anti-stress nutrients, especially magnesium and vitamins A and
E.
References
1. Meerson, F.Z. “The role of stress in the mechanism of long-
term adaptation, and prevention of stress-related injuries,” transla-
tion and summary available, Ray Peat’s Newsletter, 3977 Dillard
Road, Eugene, OR 97405.
2. Cleary, M.P., Shepherd, A., and Jenks, B. “Effect of DHEA
on growth in lean and obese Zucker rate,” J. Nutr. 114(7): 1242-
1251; 1984.
3. Coleman, D.L., Leister, E. H., and Applezweig, N.. “Thera-
peutic effects of DHEA metabolites in diabetes mutant mice,” Endo-
crinology 115(1): 239-243; 1984.
4. Rosenfeld, A. “Superpowder,” Omni magazine; 1980.
Posted in General.
Comments Off on Hormone Balancing: Natural Treatment and Cure for Arthritis
– October 15, 2011
Multiple Sclerosis & Other Hormone-Related Brain Syndromes
by Ray Peat, PhD
This article, from about 1994, gives more background, relating to the effects of estrogen; hypothyroidism typically increases adrenalin, estrogen, serotonin, and prolactin, and the estrogen difference probably accounts for why the incidence is two or three times higher in women than in men. Recent figures show that the ages from 45 to early fifites are when it’s most likely to appear in women, and that’s when progesterone is most likely to be failing, leaving estrogen unopposed.
Since I am trying to discuss a complex matter in a single article, I have separately outlined the essential technical points of the argument in a section at the beginning, then I explain how my ideas on the subject developed, and finally there is a glossary. If you start with “Short-day brain stress,” “Estrogen’s effects,” and “Symptoms and therapies,” you will have the general picture, and can use the other sections to fill in the technical details.
The Argument:
The hormones pregnenolone, thyroid, and estrogen are involved in several ways with the changes that occur in multiple sclerosis but no one talks about them.
The process of myelination is known to depend on the thyroid hormone. The myelinating cells are the oligodendroglia (oligodendrocytes) which appear to stop functioning in MS (and sometimes to a milder degree in Alzheimer’s disease, and other conditions). The cell’s absorption of thyroid hormone is influenced by dietary factors.
The oligodendrocytes are steroid-producing cells,( 1) and steroidogenesis is dependent on thyroid hormone, and on thyroid-dependent respiratory enzymes and on the heme-enzyme P-450 scc, which are all sensitive( 2) to poisoning by carbon monoxide and cyanide The steroid produced by the oligodendrocytes is pregnenolone, which is known to have a profound anti-stress action,( 3) and which appears to be the main brain-protective steroid.
Lesions resembling those of MS can be produced( 4) experimentally by carbon monoxide or cyanide-poisoning. The lesions tend to be associated with individual small blood vessels and are likely to contain clots. (Since all animals have enzymes to detoxify cyanide, this poison is apparently a universal problem and can originate in the bowel. “Detoxified” cyanide is still toxic to the thyroid.)
Pregnenolone and pogesterone protect against nerve damage( 5) by the excitotoxic amino acids (glutamic acid, aspartic acid, monosodium glutamate, aspartame, etc.), while estrogen( 6) and cortisol( 7) are nerve-destroying, acting through the excitotoxic amino acids. Excitotoxins destroy certain types of nerve, especially the dopaminergic and cholinergic types, leaving the noradrenergic types,(8) paralleling the changes that occur in aging. The clustering of oligodendrocytes around deteriorating nerve cells could represent an adaptive attempt to provide pregnenolone to injured nerve cells.
The involvement of hormones and environmental factors probably accounts for the intermittent progress of multiple sclerosis. To the extent that the environmental factors can be corrected, the disease can probably be controlled.
Short-Day Brain Stress
Shortly after I moved from Mexico to Montana, one of my students, a 32-year old woman, began having the same sensory symptoms her older sister had experienced at the same age, at the onset of multiple sclerosis Vertigo and visual distortions of some sort made her consider withdrawing from the university. I’m not sure why she tried eating a whole can of tuna for lunch a couple of days after the onset of symptoms, but it seemed to alleviate the symptoms, and she stayed on a high protein diet and never had a recurrence. She told me some of the lore of MS: That it mostly affects young adults between the ages of 20 and 40, that it is common in high latitudes and essentially unknown in the tropics, and that it is sometimes exacerbated by pregnancy and stress. (Later, I learned that systemic lupus erythematosis and other “auto-immune” diseases also tend to occur mainly during the reproductive years).
Having enjoyed the mild climate of Mexico, I became very conscious of the harm done to us by northern winters, and began developing the idea of “winter sickness.” In 1966-67 allergies, PMS, weight gain, colitis, and arthritis came to my attention as winter-related problems, and I assumed that the high-latitude incidence of MS related to what I was seeing and experiencing. Studies in Leningrad began revealing that mitochondria are injured during darkness, and repaired during daylight. I observed that hamsters’ thymus glands shrank in the winter and regenerated in the summer; shrinkage of the thymus gland is a classical feature of stress, and usually reflects the dominance of cortisone, though estrogen and testosterone also cause it to shrink. Winter’s darkness is stressful in a very fundamental way, and like any stress it tends to suppress thyroid function. In the hypothyroid state, any estrogen which is produced tends to accumulate in the body, because of liver sluggishness.
I began to see that PMS could be controlled by certain things — extra light, supplements of sodium and magnesium, high quality protein, and correction of deficiencies of thyroid and progesterone. In working on my dissertation, I saw that tissue hypoxia (lower than optimal concentrations of oxygen in the blood) may result from estrogen excess, vitamin E deficiency, or aging. There is a close biological parallel between estrogen-dominance and the other hypoxic states, such as stress/shock, and aging.
Estrogen’s Effects
As an amateur portrait painter, I had been very conscious of the blue aspect that can often be seen in the skin of young women. In pale areas, the color may actually be blue, and in areas with a rich supply of blood, such as the lips, the color is lavender during times of high estrogen influence — around ovulation and puberty, for example. During these times of estrogen dominance, the blood is not only poorly oxygenated, but it has other special properties, such as an increased tendency to clot. The Shutes’ work in the 1930s began with the use of vitamin E to antagonize estrogen’s clot-promoting tendency, and led them to the discovery that vitamin E can be very therapeutic in heart disease. More recently, it has been found that men with heart disease have abnormally high estrogen,( 9) that women using oral contraceptives have higher mortality from heart attack,( 10) and that estrogen tends to promote spasm of blood vessels.( 11) (These reactions are probably related to the physiol ogy of menstruation, in which progesterone withdrawal causes spasms in the spiral arteries of the uterus, producing endometrial anoxia and cell death.)
In toxemia of late pregnancy, or eclampsia, the exaggerated clotting tendency caused by excess estrogen (or by inadequately opposed estrogen, i.e., progesterone deficiency), can cause convulsions and strokes. Vascular spasms could be involved here, too. The stasis caused by the vasospasm would facilitate clotting. (Vascular spasm has been observed in epilepsy, too. Epilepsy can be brought on by the premenstrual excess of estrogen, and in that situation there is no evidence that clotting is involved. Leakage of hemoglobin out of red cells can cause vasospasm, so bleeding, clotting, strokes, and seizures can interact complexly.) The brains of women who have died following eclampsia show massive clotting in the blood vessels, and their livers are characteristically injured, with clots.( 12)
Tom Brewer and others have shown very clearly that malnutrition, especially protein deficiency, is the cause of toxemia of late pregnancy.
Various researchers have demonstrated that the plaques of MS usually occur in the area served by a single blood vessel,( 13, 14) and some have suggested that clotting is the cause. MS patients have been found to have an abnormal clotting time, and it has been suggested that an altered diet might be able to correct the clotting tendency.
Studies in animals have shown clearly that a protein deficiency increases the fibrinogen content of blood. (Field and Dam, 1946.) Other factors that increase blood clotting are elevated adrenaline and cortisone. Protein deficiency causes an adaptive decrease in thyroid function, which leads to a compensatory increase in adrenaline and cortisone. The combination of high estrogen with high adrenaline increases the tendency for both clots and spasms of the blood vessels.( 11)
In experimental poisoning of animals with carbon monoxide or cyanide, the brain lesions resembling MS include blood clots. The patchy distribution of these spots in the brain suggests that the clotting is secondary to metabolic damage in the brain. Presumably, the same would be true in ordinary MS, with clots and spasms being induced in certain areas by metabolic abnormalities in brain cells. The injured cells that are responsible for myelination of nerve fibers are steroid-forming cells. A failure to secrete their protective pregnenolone could cause a local spasm of a blood vessel. The circulatory problem would exacerbate the respiratory problem. Steroid production is dependent on NADH and NADPH, and so requires adequate energy supplies and energy metabolism. The phenomenon of blood-sludging, studied by M. Knisely at the University of Chicago in the 1930s and 1940s, is apparently a general result of decreased energy metabolism, and is likely to be a factor in energy-and-circula tory vicious circles.
Symptoms and Therapies
Around 1976 I met a woman in her mid-30s who heard about my work with progesterone in animals. She had been disabled by a brain disease that resembled MS or Devic’s disease, inflammation of the optic nerves. It would sometimes cause blindness and paralysis that persisted for weeks at a time. During remissions, sometimes using a wheelchair, she would go to the medical school library to try to understand her condition. She came across Katherina Dalton’s work with progesterone, and convinced a physician to give her a trial injection. Although she had trouble finding people who were willing to give her progesterone, her recovery was so complete that she was able to climb stairs and drive her car, and she came to my endocrinology class and gave a very good (and long) lecture on progesterone therapy. Although her sensory and motor functions became normal, she remained very fat, and chronically suffered from sore areas on her arms and legs that seemed to be abnormal blood vessels, pos sibly with phlebitis. She appeared to need thyroid hormone as well as larger amounts of progesterone, but never found a physician who would cooperate, as far as I know.
In the late 1970s I was seeing a lot of people who had puzzling health problems. In a period of two or three years, there were five people who had been diagnosed by neurologists as having Multiple Sclerosis. In talking to them, it seemed clear that they had multiple symptoms of hypothyroidism. They weren’t severely disabled. Since they weren’t fat or lethargic, their physicians hadn’t thought they could be hypothyroid. When they tried taking a thyroid supplement, all of their symptoms disappeared, including those that had led to their MS diagnosis. One of the women went to her doctor to tell him that she felt perfectly healthy since taking thyroid, and he told her to stop taking it, because people who have MS need a lot of rest, and she wouldn’t get enough rest if she was living in a normally active way. The assumption seemed to be that the diagnosis was more important than the person. (When I refer to a “thyroid supplement” I mean one that contains some T3. Many people experien ce “neurological symptoms” when they take thyroxine by itself. Experimentally, it has been found to suppress brain respiration, probably by diluting the T3 that was already present in the brain tissue.)
Metabolism of the Oligodendrocytes
The rate-regulating step in steroid synthesis involves the entry of cholesterol into the mitochondria, where the heme-enzyme P-450 scc then removes the side-chain of cholesterol (by introducing oxygen atoms), to produce pregnenolone. This enzyme can be poisoned by carbon monoxide or cyanide, and light can eliminate the poison;( 18) this could be one aspect of the winter-sickness problem.
Peripheral nerves are myelinated by essentially the same sort of cell that is called an oligodendrocyte in the brain, but outside the brain it is called a Schwann cell. It is easier to study the myelin sheath in peripheral nerves, and the electrical activity of a nerve is the most easily studied aspect of its physiology. Certain experiments seemed to indicate a “jumping” (saltatory) kind of conduction along the nerve between Schwann cells, and it was argued that the insulating function of the myelin sheath made this kind of conduction possible. This idea has become a standard item in physiology textbooks, and its familiarity leads many people to assume that the presence of myelin sheaths-in the brain serves the same “insulating” function
For a long time it has been known that heat production during nerve conduction reveals a more continuous mode of conduction, that doesn’t conform to the idea of an electrical current jumping around an insulator. Even if the myelin functioned primarily to produce “saltatory conduction” in peripheral nerves, it isn’t clear how this process could function in the brain. I think of the issue of “saltatory conduction at the nodes of Ranvier” as another of the fetish ideas that have served to obstruct progress in biology in the United States. A more realistic approach to nerve function can be found in Gilbert Ling’s work. Ling has demonstrated in many ways that the ruling dogma of “cell membrane” function isn’t coherently based on fact. He found that hormones such as progesterone regulate the energetic and structural stability of cells. Many people, unaware of his work, have felt that it was necessary to argue against the idea that there are anesthetic steroids with generalized protect ive functions, because of their commitment to a textbook dogma of “cell membrane” physiology.
I think the myelinating cells do have relevance to nerve conduction, but I don’t think they serve primarily as electrical insulators. If the adrenal cortex were inside the heart, it would be obvious to ask whether its hormones aren’t important for the heart’s function. Since the oligodendrocytes are steroid-synthesizers, it seems obvious to ask whether their production of pregnenolone in response to stress or fatigue isn’t relevant to the conduction processes of the nerves they surround.
Old Age
A biologist friend of mine who was about 85 became very senile. His wife started giving him thyroid, progesterone, DHEA and pregnenolone, and within a few days his mental clarity had returned. He continued to be mentally active until he was 89, when his wife interfered with his access to the hormones.
In old age the brain steroids fall to about 5% of their level in youth. Pregnenolone and DHEA improve memory in old rats, and improve mood stability and mental clarity of old people. Pregnenolone’s action in improving the sense of being able to cope with challenges probably reflects a quieting and coordinating of the “sequencing” apparatus of the forebrain, which is the area most sensitive to energy deprivation. This is the area that malfunctions in hyperactive and “dyslexic” children. Weakening of the sequencing and sorting processes probably explains the common old-age inability to extract important sounds from environmental noise, creating a kind of”confusion deafness.” Insomnia, worry and “restless legs” at bedtime are problems for many old people, and I think they are variations of the basic energy-depletion problem.
The oligodendrocytes were reported (Hiroisi and Lee, 1936) to be the source of the senile plaques or amyloid deposits of Alzheimer’s disease.( 16) Hiroisi and Lee showed the cells in different stages of degeneration, ending with translucent “mucoid” spots that stained the same as amyloid, the material in the senile plaques. This type of cell also appears to form a halo or crown around degenerating nerve cells — possibly in a protective reaction to provide the nerve cell with any pregnenolone the oligodendrocytes are able to make. The oligodendrocytes, the source of the brain steroids (that people previously believed came from the adrenals and gonads, and were just stored in the brain), myelinate nerve fibers under the influence of thyroid hormone.( 17) Thyroid is responsible for both myelination and hormone formation. In old age, glial cells become more numerous, and nerve cells become structurally and functionally abnormal, but usually there is no problem with the formation of m yelin. In MS, the problem is just with myelination, and there are no senile plaques or defects in the nerve cells themselves.
These differences suggest the possibility that Alzheimer’s disease involves a specific premature loss of brain pregnenolone production, but not of thyroid. Recent work suggests a central role for pregnenolone and progesterone in the regulation of consciousness,( 18) and possibly in the brain’s detoxifying system. Elsewhere, I have suggested that vitamin A deficiency might cause the excessive production of the “amyloid” protein. A vitamin A deficiency severely inhibits steroid synthesis. (It is used so massively in steroid synthesis that a progesterone supplement can prevent the symptoms of vitamin A deficiency.) I suspect that vitamin A is necessary for the side-chain cleavage that converts cholesterol to pregnenolone. Iron-stimulated lipid peroxidation is known to block steroid formation, and vitamin A is very susceptible to destruction by iron and oxidation. Iron tends to accumulate in tissues with aging. Gajdusek has demonstrated that brain deterioration is associated with the retention of whatever metal happens to be abundant in the person’s environment, not just with aluminum. (One type of glial cell is known for its metal-binding function, causing them to be called “metallophils.”) According to Gajdusek, “calcium and other di- and trivalent elements” are “deposited as hydroxyapatites in brain cells” in brain degeneration of the Alzheimer’s type.( 19)
Even early forms of Alzheimer’s disease begin at an age when the youth-associated steroids have begun to decline. If MS involves a deficiency of thyroid (or of T3 within the oligodendrocytes, where T3 normally can be made from thyroxine; many things, including protein deficiency, can block the conversion of T4 to T3), those cells would necessarily be deficient in their ability to produce pregenolone, but in young people the brain would still be receiving a little pregnenolone, progesterone, and DHEA from the adrenals and gonads. This relatively abundant youthful supply of hormones would keep most of the body’s organs in good condition, and could keep the bodies of the major brain cells from deteriorating. But if proper functioning of the nerve fibers requires that they be fed a relatively high concentration of pregnenolone from their immediately adjacent neighbors (with the amount increasing during stress and fatigue), then their function would be impaired when they had to depen d on the hormones that arrived from the bloodstream.
For many years it has been recognized that the brain atrophy of “Alzheimer’s disease” resembles the changes seen in the brain in many other situations: The traumatic dementia of boxers; toxic dementia, the slow-virus diseases; exposure of the brain to x-rays;( 20) ordinary old age; and in people with Down’s syndrome who die around the age of thirty.
In menopause, certain nerve cells have lost their ability to regulate the ovaries, because of prolonged exposure to estrogen.( 6) The cells that fail as a result of prolonged estrogen exposure aren’t the same cells that fail from prolonged exposure to the glucocorticoids,( 7) but they have in common the factor of excitatory injury.
Since people who experience premature menopause are known to be more likely than average to die prematurely, it is reasonable to view menopause as a model of the aging process. It is now well established that progesterone fails to be produced at the onset of menopause (the first missed period, increased loss of calcium, symptoms such as hot flashes, etc.), and that estrogen continues to be produced at monthly intervals for about four years. The essential question for aging, in the present context, is why the anesthetic steroids are no longer produced at a rate that allows them to protect tissues, including brain cells, from the excitotoxins. Using menopause as a model for aging, we can make the question more answerable by asking why progesterone stops being produced.
During stress, we are designed not to get pregnant, and the simplest aspect of this is that ACTH, besides stimulating the adrenals to produce stress-related hormones, inhibits the production of progesterone by the ovary. Other stress-induced factors, such as increased prolactin and decreased thyroid, also inhibit progesterone production. Stress eventually makes us more susceptible to stress. Menopause and other landmarks of aging simply represent upward inflections in the rate-of-aging curve. Individual variations in type of stress, hormonal response and diet, etc., probably govern the nature of the aging process in an individual.
The amphetamine-like action of estrogen, which undoubtedly contributes to the general level of stress and excitotoxic abuse of nerve cells, is probably the only “useful” facet of estrogen treatment, but a little cocaine might achieve the same effect with no more harm, possibly less. The toxicity of catecholamines has been known for over 30 years, and conversion to catechol-estrogens which increase the activity of brain catecholamines. Estrogen’s powerful ability to nullify learning seems never to be mentioned by the people who promote its use. The importance of a good balance of brain steroids for mood, attention, memory, and reasoning is starting to be recognized, but powerful economic forces militate against its general acceptance.
Since the brain is the organ that can allow us to adapt without undergoing stress in the hormonal sense, it is very important to protect its flexibility and to keep its energy level high, so it can work in a relaxed way. It is the low energy cellular state that leads to the retention of calcium and iron, and to the production of age pigment, and other changes that constitute the vicious circle of aging. And mental activity that challenges obsession and rigidity might be the most important brain energizer. Pseudo-optimism, humor-as-therapy, has a certain value, but a deeper optimism involves a willingness to assimilate new information and to change plans accordingly.
Supplements
Nutritional supplements that might help to prevent or correct these brain syndromes include: Vitamin E and coconut oil; vitamin A; magnesium, sodium; thyroid which includes T3; large amounts of animal protein, especially eggs; sulfur, such as magnesium sulfate or flowers of sulfur, but not to take continuously, because of sulfur’s interference with copper absorption; pregnenolone; progesterone if needed. Bright light, weak in the blue end of the spectrum and with protection against ultraviolet, activates respiratory metabolism and quenches free radicals. Raw carrot fiber and/or laxatives if needed; charcoal occasionally for gas or bowel irritation. Coconut oil serves several purposes. Its butyric acid is known to increase T3 uptake by glial cells. It has a general pro-thyroid action, for example by diluting and displacing antithyroid unsaturated oils, its short-and medium-chain fatty acids sustain blood sugar and have anti-allergic actions, and it protects mitochondria against s tress injury.
In 1979, a woman whose husband was suffering from advanced Amyotrophic Lateral Sclerosis (ALS) asked me if I had any ideas for slowing his decline. I described my suspicion that ALS involved defective metabolism or regulation of testosterone. In some tissues, testosterone is selectively concentrated to prevent atrophy, and ALS is a disease of middle-age, when hormone regulation often becomes a special problem. In the late 1970s, there was discussion of a higher incidence of ALS in males, and especially in athletes I told her about progesterone’s general protective effects, its antagonism to testosterone, and its prevention of atrophy in various tissues. She decided to ask her doctor to try progesterone for her husband Later, I learned that her husband had gone into a very rapid decline immediately after the injection, and died within a week; the physician had given him testosterone, since, he said, “testosterone and progesterone are both male hormones.” Besides making me more aware of the problems patients have in communicating with physicians, this tended to reinforce my feeling that a hormone imbalance is involved in ALS. Although I haven’t written much about testosterone’s toxicity, Marian Diamond’s work showed that prenatal testosterone is similar to prenatal estrogen, in causing decreased thickness of the cortex of the brain; both of those hormones oppose progesterone’s brain-protecting and brain-promoting actions.
References
(1.) Z.Y. Hu, et al., P.N.A.S. (USA) 84, 8215-9, 1987.
(2.) P.F. Hall, Vitamins and Hormones 42, 315-370, 1985.
(3.) J.J. Lambert, et al., Trends in Pharmac. Sci. 8, 224-7, 1987.
(4.) W.A.D.A. Anderson, Pathology (second edition), C.V. Mosby, St. Louis, 1953.
(5.) S.S. Smith, et al., Brain Res. 422, 52-62, 1987.
(6.) P.M. Wise Menopause, 1984; S.S. Smith, et al., Brain Res. 422, 40-51, 1987.
(7.) R.M. Sapolsky, et al., J. Neuroscience 5, 1222-1227, 1985; R.M. Sapolsky and W. Pulsinelli, Science 229, 1397-9, 1985.
(8.) C.B. Nemeroff, (Excitetoxins) 290-305, 1984.
(9.) G.B. Phillips, Lancet 2, 14-18, 1976; G.B. Phillips, et al., Am. J. Med. 74, 863-9, 1983; M.H. Luria, et al.,Arch Intern Med 142, 42-44, 1982; E.L. Klaiber, et al., Am J Med 73,872-881, 1982.
(10.) J.I. Mann, et al., Br. Med J 2, 241-5, 1975.
(11.) V. Gisclard and P.M. Vanhoutte, Physiologist 28, 324 (48.1).
(12.) W.A.D.A. Anderson, Pathology, 1953; H.H. Reese, et al., editors, 1936 Yearbook of Neurology, Psychiatry, and Endocrinology, Yearbook Publishers, Chicago, 1937.
(13.) T.J. Putnam, Ann Int Med 9, 854-63, 1936; JAMA 108, 1477, 1937.
(14.) R.S. Dow and G. Berglund, Arch Neurol and Psychiatry 47, 1, 1992.
(15.) R.W. Estabrook, et al., Biochem Z. 338, 741-55, 1963.
(16.) S. Hiriosi and C.C. Lee, Arch Neurol and Psychiat 35,827-38, 1936.
(17.) J.J. Matthieu, et al., Ann Endoc. 1974.
(18.) K. Iwaharhi, et al., J Ster Biochem and Mol Biol 44(2), 163-4, 1993.
(19.) D.C. Gajdusek, Chapter 63, page 1519 in Virology (B.N. Fields, et al., editors), Raven Press, N.Y., 1985.
(20.) K. Lowenberg-Scharenberg and R.C. Bassett, J. Neuropath and Exper Neurol 9, 93, 1950.
Glossary
Amyloid is the old term for the “starchy” appearing (including the way it stains) proteins seen in various diseases, and in the brain in Alzheimer’s disease.
Cytochrome P450 scc. The cytochromes are “pigments,” in the same sense that they contain the colored “heme” group that gives hemoglobin its color. P450 means “protein that absorbs light at a wavelength of 450.” The scc means “side-chain cleaving,” which refers to the removal of the 6 carbon atoms that distinguish cholesterol from pregnenolone. Other Cyt P450 enzymes are important for their detoxifying oxidizing action, and some of these are involved in brain metabolism.
Glial means “glue-like,” and glial cells are mostly spidery-shaped cells that used to be thought of as just connective, supportive cells in the brain.
Mitochondria (the “thread-like bodies”) are the structures in cells which produce most of our metabolic energy by respiration, in response to the thyroid hormones.
Mucoid refers to a mucoprotein, a protein which contains some carbohydrate. A glycoprotein, usually not intended as a precise term.
Myelination. Myelin is a multilayered enclosure of the axons (the long processes) of nerve cells, composed of proteins and complex lipids, including cholesterol. The layered material is a flat, thin extension of the cytoplasm of the oligodendroglial cells.
Oligodendrocytes are one of the kinds of glial (or neuroglial) cells, and structurally they are unusual in having sheet-like, rather than just thread-like processes; they have a sensitivity (“receptors”) to stress and valium, and produce pregnenolone when activated. Under the influence of thyroid hormone, they wrap themselves in thin layers around the conductive parts of nerve cells, leaving a multilayered “myelin” coating. Their absorption of thyroid hormone is promoted by butyrate, an anti-stress substance found in butter and coconut oil.
Steroidogenesis is the creation of steroids, usually referring to the conversion of cholesterol to hormones.
Townsend Letter for Doctors & Patients.
Posted in General.
Comments Off on Multiple Sclerosis & Other Hormone-Related Brain Syndromes
– October 15, 2011